Precautionary allergen labelling needs a revamp
- Like
- Digg
- Del
- Tumblr
- VKontakte
- Buffer
- Love This
- Odnoklassniki
- Meneame
- Blogger
- Amazon
- Yahoo Mail
- Gmail
- AOL
- Newsvine
- HackerNews
- Evernote
- MySpace
- Mail.ru
- Viadeo
- Line
- Comments
- Yummly
- SMS
- Viber
- Telegram
- Subscribe
- Skype
- Facebook Messenger
- Kakao
- LiveJournal
- Yammer
- Edgar
- Fintel
- Mix
- Instapaper
- Copy Link
Posted: 9 October 2020 | Bethan Grylls (New Food) | No comments yet
Lynne Regent, CEO of the Anaphylaxis Campaign, tells New Food’s Bethan Grylls why we need legislation around precautionary allergen labelling.
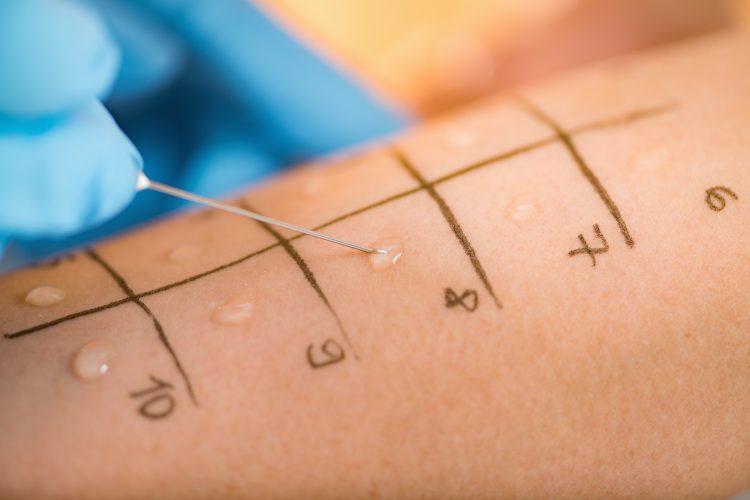

Globally, anaphylaxis results in a significant number of deaths every year. In the UK alone (which is among the top three countries with the highest incident of allergy1), an estimated 20 deaths are reported annually.2
What is anaphylaxis?
Anaphylaxis is a severe allergic reaction that occurs when an individual encounters something they are allergic to, with food as the most common cause of such a reaction.3
The reaction is unpredictable, usually occurring within minutes but it can happen up to two or three hours later. The whole body is affected with varied symptoms that often include nausea, rashes, swelling of the throat and mouth, and ultimately collapse and unconsciousness.
This kind of reaction is caused by a sudden release of chemical substances, including histamine, from cells in the blood and tissues where they are stored. This is trigged by the reaction between the allergic antibody (IgE) and the allergen, causing swelling and a fall in blood pressure.1
There were 43 ways in which labels expressed may contain.
Presently, there is no cure for allergies or anaphylaxis – and, according to the Anaphylaxis Campaign, allergies have been on the rise. There is no single, determined cause for this, but the following may be related to this increase:
- Biological inheritance
- Eating habits
- Early exposure to allergens
- Antibiotics
- Vitamin D deficiency and other dietary factors.
Anxiety and allergies
Research has found that those living with allergies may also suffer with anxiety.4 In fact, up to one in five people live in fear of death from a possible anaphylactic shock.5 But anxiety also takes other forms, including fear of social rejection and humiliation, or the expense of meal preparation and the concerns around having to carry adrenaline auto-injectors such as EpiPen or Jext.
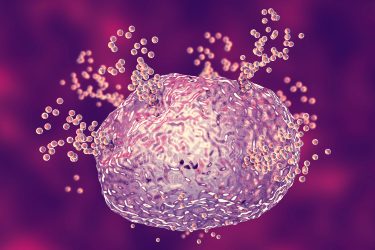

Mast cell releasing histamine during allergic response
Arguably, the use of language on products may be a contributor to this anxiety, due to the confusion it can cause among allergy sufferers and parents of children with allergies. A few years ago, the Anaphylaxis Campaign undertook research into allergen labelling, discovering that there were 43 ways in which labels expressed ‘may contain’.
“It is better now,” said Lynne Regent, CEO at Anaphylaxis Campaign, “but it’s not as good as it needs to be. We need to keep it simple; a product should read ‘may contain’ or ‘not suitable for…’
“But some insist on putting things like ‘made on a line, made in a factory…’, which mean nothing to the consumer because they cannot assess the risk based on such statements.”
May contain and legislation
There is currently no legislation around precautionary allergen labelling (PAL). “May contain is a voluntary label, used in instances where there’s a risk the ingredient/s has entered the product inadvertently,” explained Regent.
“The problem is that you can have two companies with the same level of risk (of allergen contamination), but one opts not to include an allergen warning because there’s no law that requires them to. It makes it very confusing for the consumer because they could assume if there’s no PAL label, there’s no risk and there very well may be.”
Equally, companies have been known to use ‘may contain’ labelling where there is blatantly no risk. Therefore, the credibility of ‘may contain’ is questionable. “Brands should not put a may contain label on a food unless they have carried out a thorough risk assessment and identified there is an actual danger. We have lots of examples where this labelling is used and it’s clearly silly; for example, a melon with a may contain nuts label on it.”
Regent explained that consumers will react in two different ways when they see a ‘may contain’ label – avoid all foods featuring a PAL, even in instances where the food will be fine, or disregard the phrase due its overuse and take the risk.
Some insist on putting things like ‘made on a line, made in a factory…’, which mean nothing to the consumer because they cannot assess the risk based on such statements.
“We need legalisation for this reason,” she urged. “Codex is looking into this and we are hopeful that something will happen. But until it does, we advise people – unless it is so obvious that it’s a silly label – to take ‘may contain’ warnings seriously.”
Regent would like to see legislation which provides uniform and standardised allergen testing thresholds and risk assessment procedures, as well as strict wording requirements. She acknowledged this could potentially limit choice among allergen sufferers but raised the point that “currently so many foods use ‘may contain’ that choice is already restricted”. It may also have the opposite effect and widen food choices, she countered. In any case, the benefit of introducing thresholds will be safer food, she noted, and that “must be the prime consideration”.
Thresholds
The threshold dose is the lowest amount of the allergen that can cause a reaction. Scientists are currently investigating these thresholds for several allergenic foods. Establishing these levels will be crucial if industry is ever to develop standardised legislation for PALs.
“Usually when food is contaminated there has been a lot of contact with that particular ingredient. That is why testing is so critical – if the proportion of the contaminant is so tiny, it may well be that you do not need a may contain label,” explained Regent.
According to the Anaphylaxis Campaign, scientists are confident they have sufficient information on threshold doses for 11 allergenic foods to enable UK regulators to provide strong guidance to food manufacturers. Those allergenic foods are peanut, milk, egg, some tree nuts (hazelnut, cashew), soy, wheat, mustard, lupin, sesame and shrimp/prawn. Information about fish and celery is being analysed.
In the UK, gluten has a legal threshold dose (no more than 20 parts per million), however, those with wheat allergies should be aware that ‘gluten‑free’ may not be safe for them to consume. This is because they may react to other wheat proteins or a product with less than 20 parts per million of gluten if a reasonable portion is consumed. The threshold for gluten-free is safe for those with coeliac disease.6
There are those who disagree with the idea of establishing thresholds on the basis that extremely small amounts of a food allergen can kill. The Anaphylaxis Campaign is of the belief, however, that the threshold will be extremely helpful to the allergic population. Although it does recognise that an allergic person’s threshold can vary day-to-day, dependant on their general health and whether they have been, for example, drinking alcohol. It is therefore debatable whether agreed thresholds would be misleading to a person who could react to a lower amount at specific times.
Scientists are confident they have sufficient information on threshold doses for 11 allergenic foods to enable UK regulators to provide strong guidance to food manufacturers.
The argument for thresholds would be that other practices which protect against different hazards within the food industry are based on the same threshold logic. In other words, there is always some risk, but it is low.
Scientists are working on the premise that there may well be individuals who are susceptible to an allergen under a threshold dose, but the reaction is likely to be mild.
VITAL
Australia and New Zealand have already established a labelling system which takes PALs into account. It is voluntary, but Regent regards it as “a step in the right direction”.
The programme, known as VITAL, assists food producers in risk assessment, ie, identifying the potential impact of allergen ‘cross contact’ (residue or other trace amount of an allergen) in each of their products. Moreover, it specifies a particular precautionary allergen statement to be used according to the level of cross contact present. The statement is ‘may be present: allergen x, allergen y’7 and must only be used where VITAL has been employed and in instances where the allergen level is present at ‘Action Level 2’. This represents a significant concentration of a cross contact allergen which could cause an adverse reaction.8
Navigating the law
“The majority of companies do understand labelling well and the legislation the UK does have is excellent,” Regent noted. “The 14 allergens are listed in bold on all products and all ingredients featured on the label.


“If companies are unsure they can always get advice, whether it is from us or Government bodies such as the Food Standards Agency (FSA).”
With regards to help for those with allergies, Regent said that she would like to see more allergen services – especially targeted at adults. “We see a lot of late onset allergies now, with people who are in their 30s and 40s developing them for the first time. If you are fortunate enough to live in certain parts of Britain there are good adult-geared allergy services, but we need more around the UK.”
Conclusion
“More needs to be done, but everything is moving in the right direction,” Regent said. “The awareness around anaphylaxis is better, and this is particularly due to the efforts of some families who have put themselves ‘out there’.”
She added, “The UK has been leading on developing legislation in Europe, so I am not worried that it will become diluted during this (Brexit) transition period.”
In terms of what businesses can do right now, Regent said it was all about training. “Before the pandemic, I spent a lot of time travelling the country, speaking to factories not just about what legalisation we have but why we have it. It is important that companies understand this.”
The Anaphylaxis Campaign hosts a number of training courses, most of which are free to complete. “Some only take about half an hour to do, but they actually help people to understand the basics of why they need to get this right,” Regent concluded.
References
- https://www.anaphylaxis.org.uk/wp-content/uploads/2015/06/Media-Toolkit_April-2016.pdf
- https://www.nice.org.uk/guidance/qs119/chapter/Introduction
- https://www.aaaai.org/about-aaaai/newsroom/news-releases/anaphylaxis#:~:text=Common%20Causes%3A%20
Food%20was%20the,drug%2C%20blood%20products%20and%20venom
- https://www.publichealth.columbia.edu/public-health-now/news/researchers-find-link-between-food-allergies-and-childhood-anxiety
- https://www.anaphylaxis.org.uk/wp-content/uploads/2015/06/Media-Toolkit_April-2016.pdf
- https://www.anaphylaxis.org.uk/knowledgebase/allergen-thresholds/
- http://allergenbureau.net/vital/
- https://www.afgc.org.au/wp-content/uploads/2019/10/FINAL-Food_Industry_Guide_to_Allergen_Management_and_Labelling_ANZ_2019_VD3.pdf
Biography


Related topics
Allergens, Contaminants, Food Safety, Free From, Packaging & Labelling, recalls, Regulation & Legislation, retail, Supermarket, The consumer







